Table of Contents
Introduction
When you think of stress, what usually comes to mind? Headaches, sleepless nights, or feeling overwhelmed? Do you ever think that stress affect gut health? Yes, stress can also impact your gut health.
Research shows that the gut and brain are closely connected, and emotional stress can disrupt the delicate balance of your digestive system. This connection is so strong that scientists often refer to the gut as the “second brain.”
In this article, we’ll explore how stress affects gut health, the role of the gut-brain axis, the impact on the gut microbiome, and practical strategies to manage stress for a healthier gut.
The Gut-Brain Connection: Why Stress Impacts Digestion
Your gut and brain communicate constantly through a network of nerves, hormones, and biochemical signals known as the gut-brain axis. The vagus nerve, the longest cranial nerve in the body, plays a major role in transmitting messages between the brain and the gut.
When you experience stress—whether it’s from work, relationships, or daily challenges—your body activates the “fight or flight” response. This response can trigger changes in the digestive system, such as:
- Reduced blood flow to the stomach and intestines
- Slower digestion or, in some cases, faster bowel movements
- Increased stomach acid production
- Alterations in the gut microbiome
These changes highlight why stress and gut health are deeply intertwined.
The Science of Stress and Digestion
To understand how stress impacts your gut, it helps to look at the stress response system.
When you’re stressed, the brain activates the hypothalamic-pituitary-adrenal (HPA) axis, releasing hormones like cortisol and adrenaline. These hormones prepare your body to fight or flee from a threat.
But here’s the catch—when stress is chronic, the constant release of cortisol disrupts digestion:
- Cortisol slows down digestion by reducing stomach and intestinal activity.
- Adrenaline diverts blood away from the gut to muscles, affecting nutrient absorption.
- Long-term stress changes how your gut bacteria grow and interact.
This explains why many people feel gut discomfort when stressed, even if they don’t have a digestive condition.
How Stress Affects the Digestive System
Stress does more than just cause a “nervous stomach.” It can lead to or worsen several digestive issues:
1. Irritable Bowel Syndrome (IBS)

IBS is one of the most common conditions linked to stress. People with IBS often experience abdominal pain, bloating, diarrhea, or constipation. Stress doesn’t directly cause IBS, but it can trigger flare-ups and worsen symptoms.
2. Stomach Ulcers and Acid Reflux

Stress may increase stomach acid production, leading to acid reflux or worsening existing ulcers. While bacteria like H. pylori play a primary role in ulcers, stress can make the condition more severe.
3. Gut Inflammation
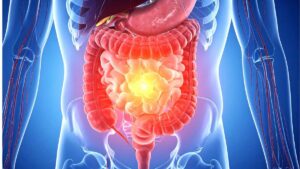
Chronic stress can weaken the immune system, increasing inflammation in the gut. This inflammation may contribute to conditions like Crohn’s disease and ulcerative colitis.
4. Changes in Appetite

Stress can affect eating habits. Some people overeat (stress eating), while others lose their appetite. Both behaviors can disrupt normal digestion and impact gut health.
Psychological Stress vs. Physical Stress

Not all stress is the same. Your gut reacts to both psychological stress and physical stress, though the triggers differ.
- Psychological stress comes from emotional factors like anxiety, trauma, or constant worry.
- Physical stress may result from illness, over-exercising, infections, or surgery.
Interestingly, both types of stress activate the same hormonal pathways, leading to gut disturbances like bloating, nausea, or diarrhea.
Hormones That Link Stress and Gut Health
The gut-brain connection relies heavily on hormones. Here are the main players:
- Cortisol: The main stress hormone. Prolonged high levels can damage the gut lining and disrupt the microbiome.
- Serotonin: Around 90% of serotonin is produced in the gut. Stress can lower serotonin production, leading to poor digestion and mood swings.
- Ghrelin & Leptin: These hormones regulate appetite. Stress disrupts their balance, leading to overeating or appetite loss.
This hormonal imbalance explains why stress can feel like both a physical and emotional burden.
Stress and the Gut Microbiome
The gut microbiome—the trillions of bacteria and microorganisms living in your intestines—plays a crucial role in digestion, nutrient absorption, and immunity. Stress can disrupt this delicate balance in several ways:
- Reduced diversity of gut bacteria: Chronic stress can decrease the variety of beneficial microbes.
- Overgrowth of harmful bacteria: Stress hormones like cortisol may create an environment where harmful bacteria thrive.
- Weakened gut barrier: Stress can increase intestinal permeability, also known as “leaky gut,” allowing toxins and bacteria to enter the bloodstream.
This imbalance in the gut microbiome can affect not only digestion but also mood, mental health, and overall well-being.
Stress and Immunity: The Gut’s Defense System
Did you know that 70% of your immune system resides in the gut? When stress weakens the gut lining and microbiome, your body’s defenses suffer.
- Chronic stress increases inflammation, which can worsen autoimmune conditions.
- A disrupted gut allows pathogens to invade, leading to infections.
- Reduced gut bacteria diversity weakens your natural immune resilience.
Managing stress isn’t just about digestion—it’s also about strengthening your immune health.
Childhood Stress and Long-Term Gut Health
Stress in early life has long-lasting effects on the gut-brain axis. Research shows that children exposed to chronic stress or trauma often have:
- Higher risks of IBS and digestive disorders in adulthood.
- Increased anxiety and depression linked to microbiome changes.
- Greater vulnerability to inflammation and food sensitivities.
This highlights the importance of nurturing stress management skills from a young age.
The Cycle of Stress and Gut Health
One of the most fascinating aspects of the gut-brain connection is that it’s a two-way street. Just as stress affects your gut, poor gut health can also influence your brain and emotions.
For example:
- An unhealthy gut microbiome may produce fewer mood-regulating neurotransmitters like serotonin.
- Gut inflammation may send distress signals to the brain, increasing anxiety and stress.
This creates a vicious cycle where stress worsens gut health, and poor gut health increases stress. Breaking this cycle is key to restoring balance.
Signs That Stress Is Affecting Your Gut
You may not always realize that stress is behind your digestive discomfort. Here are some common signs to watch for:
- Frequent stomach aches or cramps
- Bloating or excessive gas
- Irregular bowel movements (constipation or diarrhea)
- Heartburn or acid reflux
- Unexplained nausea
- Sudden changes in appetite
If these symptoms occur during stressful times, your gut may be signaling that stress is taking a toll.
Stress Management for Gut Health
The good news is that managing stress can greatly improve your gut health. Here are some proven strategies:
1. Mindfulness and Meditation

Practicing mindfulness helps calm the nervous system and reduce stress hormones. Even 10 minutes of meditation daily can improve both mental and digestive health.
2. Exercise Regularly

Physical activity reduces stress and stimulates healthy gut motility. Activities like yoga, walking, and swimming are especially effective for balancing the gut-brain connection.
3. Balanced Diet for Gut Health

Eating a diet rich in fiber, prebiotics, and probiotics supports a healthy gut microbiome. Foods like yogurt, kefir, sauerkraut, bananas, and oats can help restore microbial balance.
4. Adequate Sleep

Poor sleep increases stress and disrupts digestion. Aim for 7–9 hours of quality sleep each night to allow your gut time to repair.
5. Deep Breathing Techniques

Slow, deep breathing activates the vagus nerve, calming the gut-brain axis and improving digestion.
6. Limit Caffeine and Alcohol

Both caffeine and alcohol can irritate the digestive tract and worsen stress-related gut issues. Moderation is key.
7. Seek Professional Help

If stress-related gut problems persist, consult a doctor or gastroenterologist. Cognitive-behavioral therapy (CBT) and stress management counseling may also be beneficial.
Foods That Support Stress and Gut Health

Diet plays a major role in maintaining a healthy gut during stressful times. Here are some gut-friendly foods:
- Fermented foods: Yogurt, kimchi, miso, kombucha (rich in probiotics)
- High-fiber foods: Beans, whole grains, leafy greens
- Omega-3 rich foods: Salmon, flaxseeds, walnuts (reduce inflammation)
- Polyphenol-rich foods: Berries, dark chocolate, green tea (support gut bacteria)
- Herbal teas: Chamomile, peppermint, ginger (calm digestion and reduce stress)
Stress-Reducing Lifestyle Habits for Gut Health

Beyond diet and exercise, other lifestyle choices can greatly reduce stress and improve digestion:
- Yoga and Gut Health: Poses like child’s pose and seated twist promote relaxation and aid digestion.
- Herbal Remedies: Natural adaptogens like ashwagandha and teas like chamomile can calm the nervous system.
- Digital Detox: Reducing screen time lowers overstimulation and mental stress.
- Time in Nature: Exposure to natural environments lowers cortisol levels and increases microbiome diversity.
Long-Term Benefits of Managing Stress for Gut Health
By reducing stress, you’ll not only protect your digestive system but also experience benefits such as:
- Fewer IBS flare-ups
- Reduced bloating and acid reflux
- Stronger immune system
- Improved mood and mental health
- More energy and vitality
A healthy gut supports nearly every aspect of your well-being, making stress management an investment in your overall health.
When to Seek Medical Help
Not all gut symptoms are “just stress.” It’s important to see a doctor if you experience:
- Persistent or severe abdominal pain
- Blood in stool
- Unexplained weight loss
- Chronic diarrhea or constipation
- Stress that interferes with daily life
Doctors may recommend medical tests, dietary adjustments, therapy, or medication to manage the root cause.
Future Research on Stress and Gut Health
The relationship between stress and gut health is a growing area of research. Scientists are exploring:
- Psychobiotics: Probiotics that may improve mood and reduce stress.
- Personalized nutrition: Diets tailored to support the microbiome under stress.
- Vagus nerve stimulation: Therapies that directly improve gut-brain communication.
The future looks promising for holistic treatments that target both stress and digestive health.
FAQs on Stress and Gut Health
1. Can stress alone cause gut problems?
Stress doesn’t directly cause conditions like ulcers or IBS but can worsen symptoms and trigger flare-ups.
2. How quickly does stress affect digestion?
In some cases, stress can impact digestion immediately (like stomach upset before a big presentation). Long-term stress has more lasting effects.
3. Does the gut really act like a “second brain”?
Yes, the gut contains over 100 million nerve cells and produces neurotransmitters like serotonin, making it highly influential on mood and mental health.
4. Can probiotics help with stress-related gut issues?
Yes, probiotics may improve gut microbiome balance and reduce stress symptoms. However, results vary, and professional guidance is recommended.
5. What’s the best way to manage stress for gut health?
A holistic approach works best—combining stress management techniques (like meditation and exercise) with a balanced diet and adequate sleep.
Final Thoughts
So, does stress affect gut health? Absolutely. Chronic stress disrupts digestion, alters the gut microbiome, and creates a cycle where poor gut health further increases stress. By understanding the gut-brain connection and taking proactive steps—like practicing mindfulness, eating gut-friendly foods, and improving sleep—you can break the cycle and support both mental and digestive health.
Remember, a calmer mind often means a healthier gut. Managing stress is not just about peace of mind; it’s about nurturing your second brain for long-term wellness.







Pingback: How Sleep Impacts Your Digestive System (Complete Guide)
Pingback: Probiotic vs Prebiotic Foods: Key Differences, Benefits & Best Sources
Pingback: How Exercise Improves Gut Health Naturally | Healthy Whizz